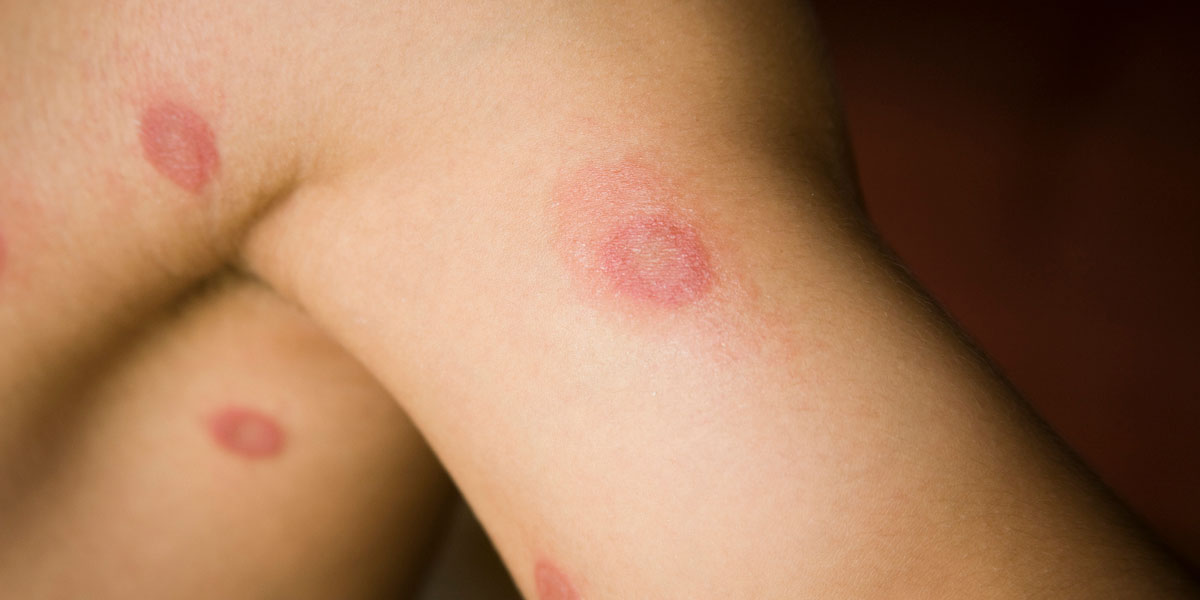
Ringworm
Not a worm, not always a ring, still a big problem

Trying to get rid of infectious for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results
What Is Ringworm?
If you’re just now learning that ringworm is a fungus, it may also surprise you to learn that it’s essentially the same thing as athlete’s foot. It’s just that when the fungi behind that source of human misery appear on other parts of the body, they go by the name of ringworm. These same fungi also cause finger- and toenail fungus infections, jock itch, and “barber’s itch”—the rash that sometimes affects men who wear beards. Since all these diseases are basically the same thing in different places, ringworm is one of the most common ailments known. According to some studies, at any one time, as much as one fifth of the population has this fungus growing on their skin and causing problems.
Ringworm: A Flesh-Eating Fungus
In other words, we’re surrounded by people carrying the disease. And that’s where the problem begins. Ringworm fungi, like all fungi, thrive by sending out chemicals that digest the substances around it. They then draw those nutrients so they can grow and reproduce. Various fungi feed on various substances, but the fungi behind ringworm feed on keratin, the main ingredient in your hair, your nails, and the dead cells that form the top layer of your skin.
So ringworm is, in a sense, a flesh-eating fungus. The good news is that it only consumes these dead cells. That means it can’t go below the skin to affect other tissue—it doesn’t even go beyond the top layer. It also doesn’t affect your mucus membranes, as in your mouth or nose.
Now for the bad news: first, your body is covered in keratin, so ringworm has plenty of room to set up shop. Second, your body is primed to fight off infection everywhere, so when your immune system detects this fungus it will react, causing redness, mild swelling, and considerable itching as it tries to fight it off. Third, if the ringworm fungus consumes enough keratin, or if scratching the itch harms the skin, it can leave the sufferer at risk for secondary infections in the manner of bug bites and poison ivy.
Ringworm Is Everywhere
There’s one more piece of bad news: the body is constantly sloughing off dead skin. And when someone carrying a ringworm fungus sheds their dead skin cells, little pieces of the fungus come off with them. These pieces can then either transfer directly to another person or lie in wait to make contact with someone else’s skin. And some ringworm fungi form spores that can survive for close to two years.
So if you’re at the gym, and your bare leg makes contact with a surface that’s been in contact with infected skin—you could pick up the fungus. If your child in daycare lies down on a mat or pillow that another child with infected skin used—your child could get ringworm, too. Some types of ringworm fungi affect pets and domestic animals. So if your cat gets infected, and you pet your cat—you could also pick up ringworm. And in all these cases, the person (or animal) doesn’t have to show active signs of infection before they become contagious.
How Do You Know When You Have Ringworm?
Still, there are distinct signs that you may have ringworm: the “ring” in the name comes from the fact that the fungus spreads outwards as it grows, pushed out from the center as it exhausts its food and as your immune system chases it down. It’s almost never a perfectly circular rash, however, and in some places—on the feet, on the scalp—it doesn’t normally form a ring at all. But if you do have a rash, here’s how ringworm distinguishes itself:
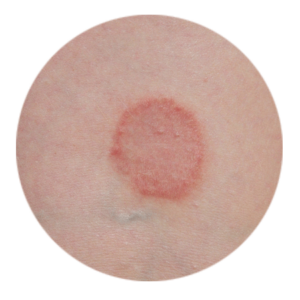
The classic presentation: As mentioned, ringworm on the chest, back, and limbs commonly appears as multiple roundish patches. The edges of the patches will be relatively sharp, will often be scaly, and will sometimes produce pus-filled sacs that resemble cellulitis; the interiors of these round patches are often clear, but sometimes they’re scaly or filled with scattered rash-like bumps. Affected skin sometimes flakes or peels, and it usually itches, burns, or stings. Note: on light skin, patches are usually tinged red; on darker skin, the patches may appear grey or brown. Note, too, that you may never get rings, but rather the rash-like bumps mentioned above.
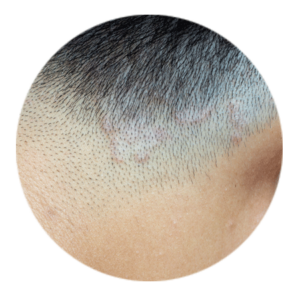
On the scalp: When it first appears, ringworm of the scalp may look like a pimple. Then the lesion may enlarge and become flaky—though it’s unlikely to form a ring. Since the fungus feeds on keratin, it can make hair fall out or become brittle (leaving a stubbly, buzz-cut-type effect in patches). Sometimes, too, a ringworm infection generates a larger pus-filled sac called a kerion. Ringworm of the scalp tends to itch as well. Note, too, that this is also how “barber’s itch”—ringworm of the beard—can show up, and it’s also how you’re most likely to experience jock itch.
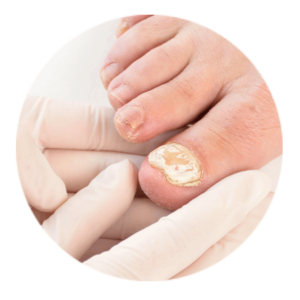
On fingernails and toenails: When ringworm affects the keratin in your finger- and toenails, the nails become brittle and ragged, and may change color to yellow or brown.

Trying to get rid of infectious for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results
What Can Put Me At Risk For Ringworm?
No question, ringworm can be a horror show. But even if the spores, or the fungus itself, gets on your skin, you’re not guaranteed an infection. Thanks to sebum and sweat, your skin is pretty acidic, making it hard for fungi (and other harmful organisms) to survive. Your skin cells are tough, too, and they resist being broken down. Also, if you maintain a good hygiene routine, you’ll probably wash off any fungus before it gains a foothold. But there are some risk factors you need to be aware of.
Environmental Risks
Moisture on the skin creates the perfect conditions for ringworm fungi, so living in a warm and humid climate, spending time in hot, humid weather, or routinely putting yourself in situations where you sweat heavily can all increase your risk of a ringworm infection.
Clothing Issues
Especially in hot weather, or under exertion, tight clothing and clothing that chafes your skin also increase the risk of infection by damaging the skin and creating the moist, warm conditions that allow the fungus to thrive.
Frequent Contact With People
People with ringworm infections can easily spread the fungus through skin-to-skin contact, so direct contact with the skin of others—through participation in a contact sport like wrestling, for example—can also boost your risk. Living in close quarters with other people increases your risk as well.
Other Underlying Illnesses
People with diabetes and people with weakened immune systems are more at risk of a ringworm infection just as a matter of course.

Watch Out for the Soil
It’s not the most common way to get ringworm, but ringworm fungi can lie dormant in the environment, especially in the soil. If you have frequent, prolonged contact with any kind of soil, you’ll want to take precautions.
Fighting Ringworm Everywhere You Find It
Even if you control for these risks, you’re not out of danger. Many ordinary activities and situations can heighten the risk of picking up a ringworm fungus. Here’s a look at those everyday risk factors, and at what you can do to confront them.
Kids in Daycare and School
From colds to lice, everyone knows that schools and daycares can be breeding grounds for disease and parasites. Schools can serve as wonderful incubators of ringworm, too. One 2010 study of elementary school students in Kansas City, for example, found that nearly 7% of the kids had ringworm scalp infections, with infection rates as high as 30% in some schools.
Fortunately, there are some simple strategies you can use to help cut down the possibility that your kids will pick up ringworm at daycare or school.
Tell kids not to share anything that’s likely to contact their skin.
Make regular bathing a habit, and encourage more frequent bathing.
If your child contracts ringworm, keep them out of school.
Be on the lookout for signs of infection.
If you’re a teacher or administrator, set all this as policy.

Trying to get rid of infectious for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results
Ringworm at the Gym
As bad as schools are for transmitting infections, gyms may be even worse. For example, a 2014 study conducted in the Memphis, TN area checked all the places where gym equipment (including elliptical trainers, treadmills, free weights, and weight machines) came in contact with members’ skin and found an ocean of bacteria at all these sites. Most of the bacterial strains were benign, but there were strains of salmonella, staph, and other harmful organisms. Since it’s well known that ringworm can lie in wait in the environment, this bacterial contamination gives a good sense of how easy it would be to find ringworm on your nearest stationary bike. Worse, with their swimming pools, steam rooms, and showers—and with the constant baths of sweat their surfaces receive—gyms frequently create the damp, warm conditions that help the fungus survive and render the skin more vulnerable to infection. But there are some precautions you can take that will make picking up ringworm less likely.

Sanitize Surfaces
Wipe any exercise equipment with a disinfectant wipe before you use it (and be sure to bring your own wipes if your gym doesn’t supply them). You can also use a towel or yoga mat to provide a barrier between your skin and any shared surfaces.

Bring Your Own Gear
On the subject of towels and yoga mats, always bring your own. Wash towels after each use, and clean your mat with a sanitizing (and, preferably, antifungal) solution after every class.

Wear Proper Foot Protection
Buy a pair of flip-flops or slides to protect your feet in damp areas like the locker room or around the pool. Everywhere else, keep your shoes on: you should never walk barefoot.

Wear Lose Clothing
Wear loose-fitting clothes that draw moisture away from the skin. And wash your gym clothes after each session.
Shower After Workouts
Shower as soon as you can after you work out, and try to find soaps with antifungal ingredients (such as dandruff shampoos). And when you dry off, do so with care, and pay special attention to your feet, toes, and groin area.

Always Wash Hair
You may be tempted not to wash your hair, but if you swim, or engage in activities that put your head in contact with shared surfaces, you really should.

Bring Clean Clothes
For every gym session bring clean clothes (clean socks and underwear especially) to change into after your post workout shower.

Avoid Contact
See an acquaintance at the gym? Try to avoid shaking hands. A long-lost friend? Try to avoid hugging. Skin-to-skin contact is one of the primary ways of contracting ringworm, especially when the two people are sweaty. And never share anything that comes in contact with another person’s skin, including towels, clothing, or razors.

Keep Damaged Skin Clean
This may seem obvious, but because damaged skin is more vulnerable to a ringworm infection, keep cuts, sores, and abrasions covered. And avoid damp areas like steam rooms and hot tubs until your skin heals.

Avoid Pools
Along similar lines, if you have a ringworm infection, avoid the pool. Chlorination should destroy any fungi that wash off your skin, but it’s not guaranteed, and you don’t want to spread the infection to others. Plus, dampening the skin can make ringworm more difficult to treat.
If you’re in charge of a gym
You’ve probably got a health-department mandated disinfectant and cleaning routine, but just as with schools, one of the best ways to cut down on ringworm transmission is to educate your members—especially since, no matter how clean you keep things, infected people could still casually pass on a ringworm fungus. Put out signage and literature about the risks. And encourage members to take action for themselves: Supply disinfectant wipes for people to use on equipment and any other shared surfaces, and encourage people to bring their own equipment (such as yoga mats) if possible.
Can I Really Catch Ringworm From My Pets?
Taking steps to avoid the risks of ringworm in public can certainly help, but there is one factor that can make ringworm relatively easy to get at home: pets. Yes, you can get ringworm from your pets. Cats are the worst: unlike dogs, cats can carry a ringworm fungus without showing any signs of infection. Perhaps for that reason, some studies have shown that as many as 13% of ringworm infections in humans may have come from cats (though it should be noted that the particular species of fungus that affects cats is harder to spread from human to human). Worse, there are other studies that indicate that from one third to three quarters of households with an infected cat end up with an infected human. Cats aren’t the only culprit, however. Dogs usually show signs of infection, but they can still pass it on to you. And a long list of domesticated animals, starting with guinea pigs and going up to horses, can transmit the fungus to their human companions. Still, one of the reasons humans have cats and dogs is to pet them. So what can you do?
- Get clear on the signs. Ringworm on furry creatures can be difficult to detect. But if an infection is showing signs, it will resemble ringworm on the scalp of a human, including dandruff-like flakes close to the skin and hair loss in circular patches. On less furry areas like a dog’s underbelly, ringworm can present more like it does on the human body, with scaly, crusty lesions.
- Avoid contact with infected animals. If your pet is diagnosed with a ringworm-type infection, or if you suspect that they are infected with ringworm, try to avoid skin-to-fur contact, however hard that is on you both. If you must touch your pet, wash your hands well afterwards, preferably with an antifungal soap.
- Keep it clean. Having a pet in the house will probably intensify your cleaning regimen anyway, but an infected pet should really get you going. Wash their bedding as often as possible, and take care to vacuum any furniture, rugs, or other surfaces your pet likes to lie on. You may, in fact, want to restrict your pet to parts of the house that are easiest to clean, such as where there are bare floors and less upholstered furniture.
You Can Get Ringworm From the Great Outdoors, Too
There’s another way you can get ringworm at home—through the soil. That’s right: just by working in the garden, you could pick up a ringworm infection. It’s a relatively rare way to get ringworm, but it does happen. After all, ringworm fungi can survive away from a human host for a long time, and especially during the summer months, your yard or garden could supply all the heat and moisture needed to keep those spores or fungi viable. Fortunately just a few common sense precautions can help keep you fungi-free.
- Avoid skin-to-soil contact. There’s a reason why so many gardeners wear gloves: in addition to reducing the contact rashes caused by toxic plants, they also protect the skin from harmful microorganisms in the soil. Gloves are, therefore, your first line of defense against ringworm fungi. But you’ll also want to protect other parts of your body. This is best done by using a kneeling mat or other barrier, and by wearing long pants when you work outdoors.
- Cleanliness is essential. You’ll get dirty gardening, of course, but it’s important to at least wash your hands once you’re done, and any other skin surfaces, like your arms or knees, that were exposed to the soil. You might consider always showering immediately after yard work in the same way you should shower after a workout at the gym.
- Be ready to fight back. Ringworm fungi will usually only be present in small patches in the soil around your house (there seems to be a connection to rodent wastes). But sometimes there can be enough of those patches to make ringworm fungus endemic in your yard. If you or your pets get infected frequently, consider treating your yard with a fungicide or taking steps to eliminate particularly damp conditions.
What To Do If You Get Ringworm
With all the risks out there, it’s no wonder ringworm is so prevalent. Fortunately, the cure is certain, if a little slow. Of course, the diagnosis comes first: Usually a dermatologist can i.d, a ringworm infection on sight, but your doctor may want to scrape off a sample of infected skin and inspect it under a microscope as well.
Once the diagnosis has been made, treatment takes several forms:
- Antifungal ointments or creams. Your dermatologist will most likely start you on a topical antifungal ointment, which you’ll have to apply to infected areas daily for at least a couple of weeks and possibly as long as a month.
- Oral antifungal medicines. If you’ve got ringworm over a large area, your doctor may prescribe an oral medicine (tablets, capsules, or liquids) that will help your body fight the infection. You’ll also probably get oral doses if you have ringworm of the scalp, a fungal nail infection, or barber’s itch. Oral medications can clear an infection in a matter of days, but a particularly widespread or recurring infection can take as long as three months to cure.
- Sprays and powders. For the harder-to treat areas, especially those that tend to stay covered, like the groin or feet, your dermatologist may tell you to use an over-the-counter antifungal spray or powder. If this doesn’t offer relief, you may be put on an oral medicine after a few weeks.
Sources
www.drfungus.org/knowledge-base/tinea-corporis-tinea-cruris-tinea-pedis/ kidshealth.org/en/parents/fungal-ringworm.html
www.oureverydaylife.com/38746-prevent-ringworm-gyms.html
www.ringworminhumans.weebly.com/
www.aad.org/media/news-releases/do-i-have-ringworm
www.aad.org/public/skin-hair-nails/skin-care/preventing-common-skin-infections-at-the-gym
www.aafp.org/afp/2003/0101/p101.html www.drgreene.com/qa-articles/ringworm-treatment/
www.emedicinehealth.com/image-gallery/ringworm_of_the_nails_picture/images.htm
www.healthline.com/health/how-long-is-ringworm-contagious
www.hunker.com/12307936/how-to-get-rid-of-ringworm-spores-in-your-yard
www.makelifenatural.net/can-swimming-worsen-ringworm/
www.mayoclinic.org/diseases-conditions/ringworm-body/symptoms-causes/syc-20353780
www.medicinenet.com/catching_ringworm_from_pets/views.htm
www.ucdavis.edu/one-health/most-common-infectious-diseases-from-pets/
www.webmd.com/children/news/20100419/ringworm-is-common-among-school-age-kids#1
www.webmd.com/skin-problems-and-treatments/ringworm-myths-facts#1

Trying to get rid of infectious for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results