This virus is currently sweeping many regions of the world, so travel to many countries now carries lower or higher risks of encountering it. To protect yourself and your family, it’s critical that you understand exactly what Zika is, where you can expect to find it, and how it is transmitted. It’s also helpful to know the signs and symptoms of the virus, as well as the best methods of prevention and the populations at highest risk.
Everything You Need to Know About the Health Risks of Zika

Trying to get rid of mosquitoes for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results
No one wants to spend a lot of time and energy planning a vacation around a possible illness. Nevertheless, the Zika virus presents significant enough health risks that it’s important to know what you’re dealing with.
What Is the Zika Virus?
This mosquito-transmitted infection is related to dengue, yellow fever, and West Nile virus. It was first discovered in Uganda’s Zika forest in 1947 and is believed to be common across Africa and Asia. It did not begin spreading widely in the Western Hemisphere until recent years, where it has been identified in 35 countries.
The virus was confirmed in May of 2015, when researchers identified it as the disease causing a rash of newborns with microcephaly.
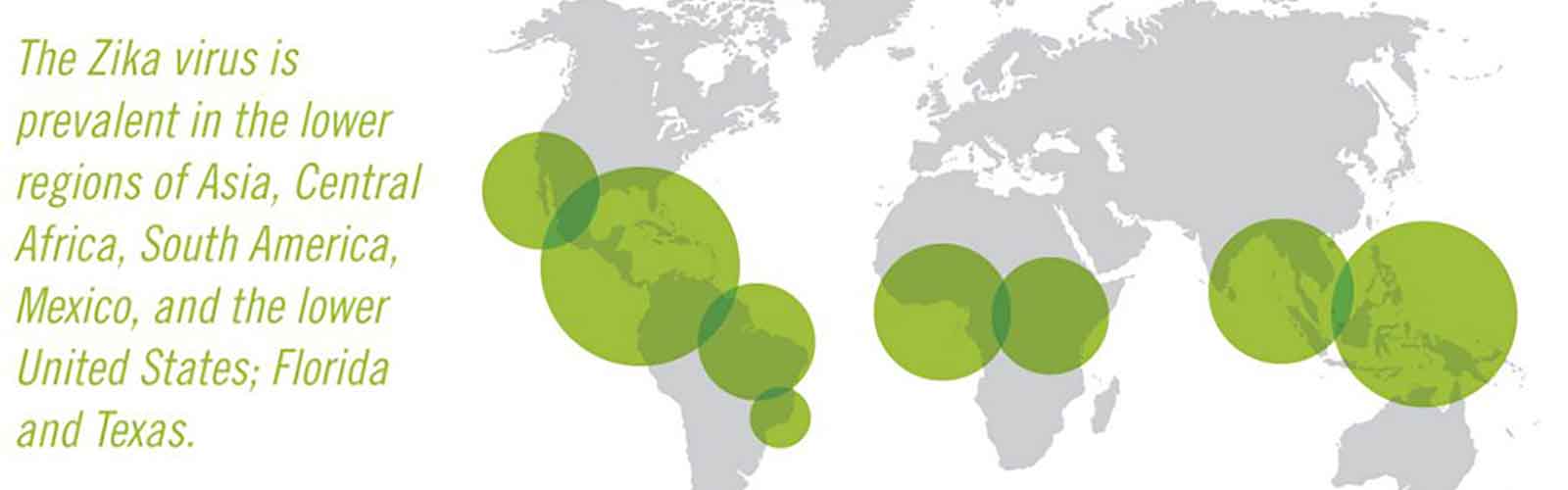
Zika Map and Areas of Occurrence
Like many mosquito-borne illnesses, the Zika virus is prevalent in the lower regions of Asia, Central Africa, much of South America, Mexico and the Caribbean Islands, and the lower United States, most notably Florida and Texas. But as of 2016, Zika has spread to other states as well, including all states along the southern border and eastern seaboard. Other areas of particular concern include Puerto Rico, Hawaii, American Samoa and the U.S. Virgin Islands. According to Live Science, the largest and highest-risk concentrations of outbreaks in the United States are in Florida, specifically Miami-Dade County.
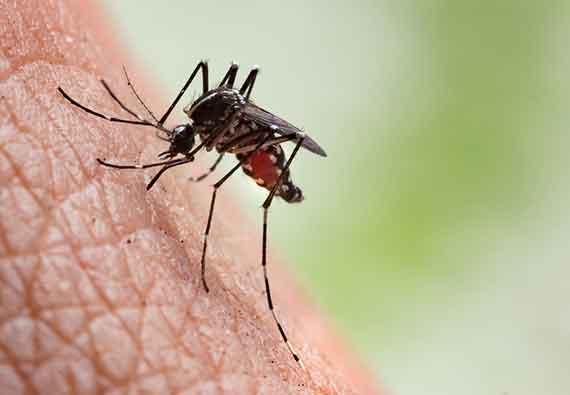
Transmission Vectors
Known as disease “vectors,” mosquitoes carry the Zika virus in their systems and deliver it to humans they bite when feeding. The infected mosquitoes are from the Aedes species, specifically Ae. aegypti and Ae. albopictus. They bite during the day and night.
Other transmission routes include pregnant women passing the virus to their fetuses, as well as men and women transmitting it to their partners during intercourse. While blood transfusion is under investigation as a possible transmission route, there have not yet been any reports that this has occurred.
No other animals are known as disease vectors for the Zika virus. Although the first case of Zika back in the 1940s was a monkey, there has since been no serious evidence suggesting that animals can develop the disease. While the Centers for Disease Control (CDC) states that nonhuman primates (apes and monkeys) have shown the ability to become infected with Zika, “only a few naturally and experimentally infected monkeys and apes have had any signs of illness at all, and then it was only a mild, transient fever without any other symptoms.”
Nor have there been any reports of Zika-infected pets. One late 1970s study done in Indonesia does offer limited evidence that horses, cows, carabaos, goats, ducks, and bats could become infected with the Zika virus. There is no evidence that these develop the disease or transmit the virus to humans, however.

Trying to get rid of mosquitoes for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results
Symptoms and Testing
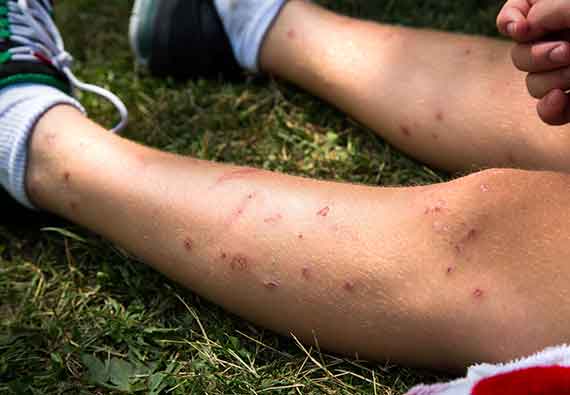
The incubation period for Zika has not been established. Researchers guess it is around a few days, as symptoms of infection usually take about that long to manifest. When symptoms do appear, they include a fever (usually a mild one), a blotchy rash (often on the chest area), conjunctivitis, pain in joints and muscles, headache, and a general feeling of being unwell. These symptoms persist for between two and seven days, and are typically no more serious than that.
These symptoms are similar to most other types of arbovirus, which, as the CDC explains, is any virus transmitted “through the bites of infected mosquitoes, ticks, sand flies or midges.” Worldwide, the most common of these viral diseases is dengue fever, with 40% of the world living in transmission zones.
Dengue fever and Zika differ in the potentially serious complications that they can cause, however. For dengue, the complications include shock and bleeding, while Zika brings with it the risk of microcephaly, a congenital abnormality, in infants who are exposed to the virus in utero. The Medical Dictionary defines microcephaly as “An abnormally small head, which is usually associated with neurodevelopmental delay and mental retardation. A standard definition is any brain or head which is ≥ 3 standard deviations below the mean for a person’s age, sex, height, weight and race.”
Another neurological disorder associated with Zika is Guillain-Barré Syndrome, defined by the National Institute of Neurological Disorders and Stroke as “a disorder in which the body’s immune system attacks part of the peripheral nervous system. The first symptoms of this disorder include varying degrees of weakness or tingling sensations in the legs. In many instances, the symmetrical weakness and abnormal sensations spread to the arms and upper body. These symptoms can increase in intensity until certain muscles cannot be used at all and, when severe, the person is almost totally paralyzed.”
Most individuals affected by this virus do not experience severe symptoms, and there is no way to be sure that someone is infected or free of Zika without lab tests on blood, urine, saliva or semen. In most cases, someone who suspects a Zika infection should follow the normal treatment for colds and flus and consult a physician if symptoms worsen.
Nevertheless, the potential complications of a Zika infection are serious enough to warrant taking precautions against contracting the disease.
Preventing the Virus
There is currently no vaccine to prevent against Zika, nor is there a medicine that specifically targets it once contracted. The Telegraph reported in June 2016, however, that researchers at the Pasteur Institute in France found that both Zika and dengue fever can be neutralized by the same antibodies, “leading to the possibility of a super-vaccine to tackle both.”
For the moment, though, the best bet for avoiding Zika is to protect yourself. Where possible, wear long pants and sleeves to avoid mosquito bites. Cover exposed areas with an insect repellent that contains DEET, IR3535 or icaridin, and always apply it according to instructions on the label.
Where possible, make use of barriers to entry into your home, hotel room, or campsite. This includes hanging mosquito netting over beds and cribs, closing doors and windows, or using screens. If you want to burn citronella candles, or use lavender or peppermint oils, be aware that these are not replacements for mosquito spray. If there is any possibility of mosquitoes entering a space, you should wear repellent at all times.
If you live in Zika transmission zones, limiting the amount of standing water helps prevent the breeding of mosquitoes. Empty water collected inside buckets, drums, clogged gutters, tires, pots, and other containers or vessels left outside. Areas of poor drainage around the house should also be eliminated.
In areas of serious concern, health and governmental authorities may advise spraying insecticides to reduce the number of mosquitoes present. Follow the rules and regulations in your area dictating what is advisable, but do not immediately begin spraying. Many insecticides are dangerous to humans and may be more likely to cause neurological or other disorders than the virus itself.
Lastly, take precautions to avoid transmitting the virus to unborn fetuses. Even monogamous couples should wear a condom at all times during a woman’s pregnancy. The CDC advises that women wait at least eight weeks and men wait at least six months after possible exposure to Zika before trying to conceive, to make sure the virus is removed from the system, even if there have been no symptoms.
High-Risk Population
Pregnant women, the highest-risk population for Zika, are advised not to travel to areas infected with the virus if it is at all possible. It is best to wait until the woman has given birth – and, ideally, until the infant is two months old and can be exposed to mosquito repellent. Non-pregnant travelers can freely visit Zika transmission zones, but they should be very careful to routinely take the precautions listed above.
Zika and Travel
Wherever you are traveling, always follow the current guidelines offered by the CDC. The organization provides very detailed guidelines for specific areas, including current guidelines for travel to Florida, so you can be aware of geographical areas experiencing severe outbreaks. If you are traveling farther afield, the CDC’s World Map of Areas with Risk of Zika will help you determine if your travel destination is vulnerable to Zika and offers detailed information for specific nations.
Also consult the U.S. Department of State’s U.S. Passports & International Travel website. This offers a full list of affected countries, as well as a list of contact numbers for more information.
No matter where you live, traveling to areas where Zika and other vector diseases are common requires caution. Keep abreast of the latest guidelines about how to protect yourself and your family. If you do, you’re far more likely to avoid serious complications and enjoy your vacation and your daily life.

Trying to get rid of mosquitoes for good?
Get a FREE Quote & BEST PRICE from a local exterminator
(866) 470-1609Available Next Day
No Obligation Assessment
Guarantee Results